 This article covers Shin Splints and is provided by Teri Burgess, resident Physiotherapist, from time-to-run Cape Town
This article covers Shin Splints and is provided by Teri Burgess, resident Physiotherapist, from time-to-run Cape Town
Shin Splints Definition and Treatment
Definition: Inflammation of the muscle attachments and interosseous membranes to the tibia (shin bone) on the inside of the front of the lower leg. Note: “shin splints” is a very widely used phrase and can refer to several lower leg injuries. The focus of this description is specifically on the inflammation described above.
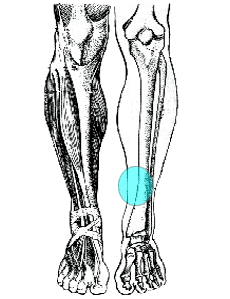
Pain or tenderness along the inside of the shin, usually about halfway down the shin. Pain and tenderness may extend to the knee
Pain on palpation of the shin
Pain is most severe at the start of a run, but may disappear during a run, as the muscles loosen up. This is different to a stress fracture, where there is pain during weight bearing activities (walking, stair-climbing)
Causes:
Inflexible calf muscles and tight Achilles tendons – place more stress on to the muscle attachments
Overpronation (feet rotate too far inward on impact) excessive running on hard surfaces, such as concrete pavements
Incorrect or worn shoes
Overtraining, or a rapid increase in training load or intensity. Beginner runners are more susceptible to this problem for a variety of reasons, but most commonly due to the fact that the leg muscles have not been stressed in such a way before they started running.
Shin Splint – Treatment Methods
Self-treatment:
Stop running, especially in the case of severe pain, if pain is mild, then reduce training load and intensity, and avoid downhill running and running on cambered surfaces
Take a course (5 – 7 days) of non-steroidal anti-inflammatory drugs(ibuprofen/voltaren/cataflam/mobic) available from your general practitioner or pharmacist
Apply ice to the shin area – for 10 minutes every 2 hours, in order to reduce the inflammation
Self-massage, using arnica oil or an anti-inflammatory gel, to the muscle only (along the inside of the shin).
Stretching of the gastrocnemius and soleus muscles. Hold for 30 secs. Relax slowly. Repeat to opposite side. Repeat stretch 2 – 3 times per day.
Remember to stretch well before running
Return to running gradually
full recovery is usually between two to four weeks
Medical treatment:
Physiotherapy, if injury doesn’t respond to self-treatment in 2 to 3 weeks
Orthotist or podiatrist for custom-made orthotics to control overpronation
Orthopaedic surgeon – if injury does not respond to physiotherapy treatment, a bone scan, diagnostic ultrasound or X-ray may be necessary to check for a stress fracture.
Alternative exercises:
swimming, pool running, cycling (in low gear) “spinning”
avoid any weight-bearing exercises
Preventative measures:
Stretching of the gastrocnemius and soleus muscles. Hold each stretch for 30 seconds, relax slowly.
Repeat stretches 2 – 3 times per day. Remember to stretch well before running.
Strengthening of foot and calf muscles.
1) Place a weight around the foot, and move your foot up and down from the ankle, with no movement in the rest of the leg. Or use a partner to grasp the foot and provide manual resistance.
2) Band exercises. Anchor one end of an exercise band (e.g; inner tubing of bicycle) to a heavy object, such as the leg of a couch. Loop the other end around the foot. Move the foot up, down, and from side to side against the band’s resistance to exercise different muscle groups.
Correct shoes, specifically motion-control shoes and orthotics to correct overpronation
Always apply ice after running
Run on soft surfaces
Avoid overstriding, which places more stress onto the shins
Gradual progression of training programme
Incorporate rest into training programme
The BIG five – the 5 most common running injuries [ in English ]
- Achilles tendonitis
- Chondromalacia – Runner’s Knee
- iliotibial band (ITB) syndrome
- Plantar Fasciitis
- Shinsplints
The BIG five – die 5 häufigsten Laufverletzungen [ auf Deutsch ]
The BIG five – Viisi yleisintä juoksuvammaa – TOP5 [ Suomeksi ]
The BIG five – De 5 vanligaste skadorna – TOP5 [ Svenska ]
adapted image credit: Running Injuries by Stephen Granger
























Trackbacks/Pingbacks